When It Comes To Stannous Fluoride, Formulation Matters
Learn more about Crest’s unique formulation of stannous fluoride dentifrice provides clinically significant improvements in gingival health, by reducing plaque quantity, toxicity, and virulence here: CLICK TO ACCESS COMPENDIUM
Backed by decades of expertise, Crest's Stannous Fluoride formulation delivers optimal gum health, longer-lasting teeth, and a superior usage experience.

*Schätzle M, et al.. J Clin Periodontol. 2003;30(10):887-901
*Biesbrock A, et al. Controlled Trials J Clin Periodontol, Dec 2019
*Biesbrock A, et al. J Periodontol, 2006; 77, 1386-1391.
*McClanahan SF, et al. J Periodontol, 2001; 72: 383-392.
*Klukowska, et al. J Clin Dent. 2017 Jun;28(2):16-26.
Expertise
Decades of innovation bring your patients over 60 years of formulating experience, over 200 U.S. patents and over 100 clinical trials. Crest Stannous Fluoride is the trusted formulation you can count on.
Efficacy
Data show significantly deeper penetration of the biofilm* and better neutralization of harmful toxins vs Colgate Total^SF† and Parodontax.
Experience
Years of consumer use make Crest Stannous Fluoride toothpaste the leader in delivering a brushing experience patients enjoy. In fact, 69% of patients who brushed with Crest Gum Detoxify wanted to brush longer.^‡
*In-Situ biofilm. †vs Colgate(R) Total^SF Whitening. ^‡Premium toothpaste users were given product information on Crest® Gum Detoxify. After 2 weeks of use, users took surveys about their experience and opinions with the product, intent to brush longer differs significantly, further studies required to measure brushing time.
Read More about The Role Of Stannous Fluoride In Maintaining Oral Health.
Crest’s Patented Stannous Fluoride Formula Treats:
Crest’s Patented Stannous Fluoride Formula Treats:
Watch How Stannous Fluoride Works
Watch our video to see how Crest Gum Detoxify works below the gumline.
See how stannous fluoride works at and below the gumline, reducing bacteria and the production of inflammatory toxins.
See the stannous fluoride molecule in action.
What Are The Consequences Of Bleeding?
Persistent Gingival Bleeding Has Long Term Oral Health Consequences
Stannous Fluoride Can Help Improve And Treat These Patient Conditions
Stannous fluoride has both bactericidal and bacteriostatic properties, which fight plaque and treat/prevent gingivitis.5,6 The stannous fluoride also deposits a protective mineral barrier over exposed dentinal tubules to help prevent sensitivity pain from triggers such as hot or cold liquids and foods.




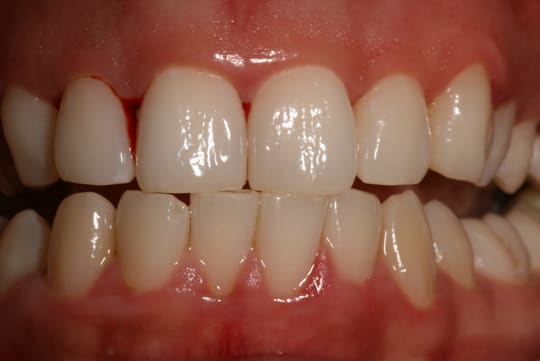 Gingivitis
Gingivitis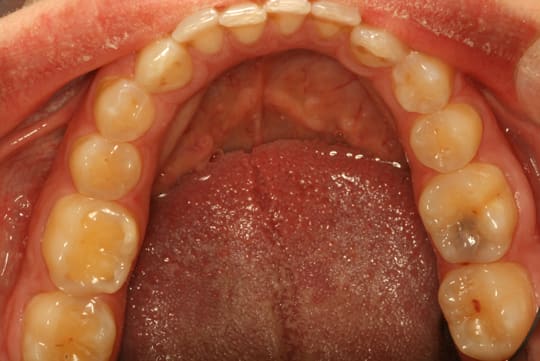 Caries
Caries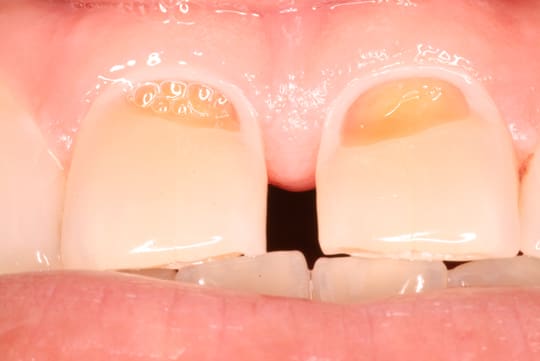 Erosion-Sensitivity
Erosion-Sensitivity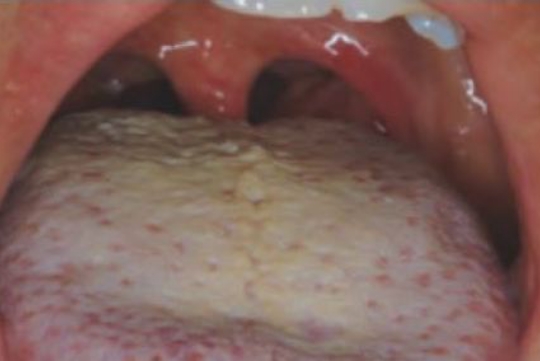 Halitosis
Halitosis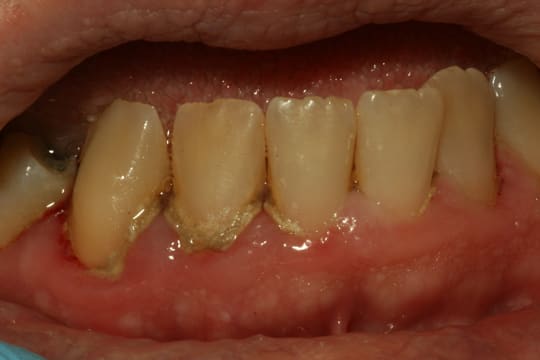 Calculus
Calculus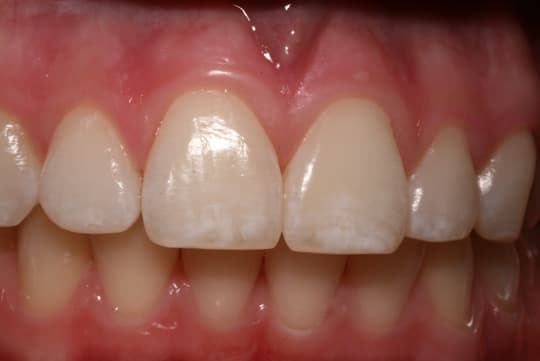 Stain Whitening
Stain Whitening






